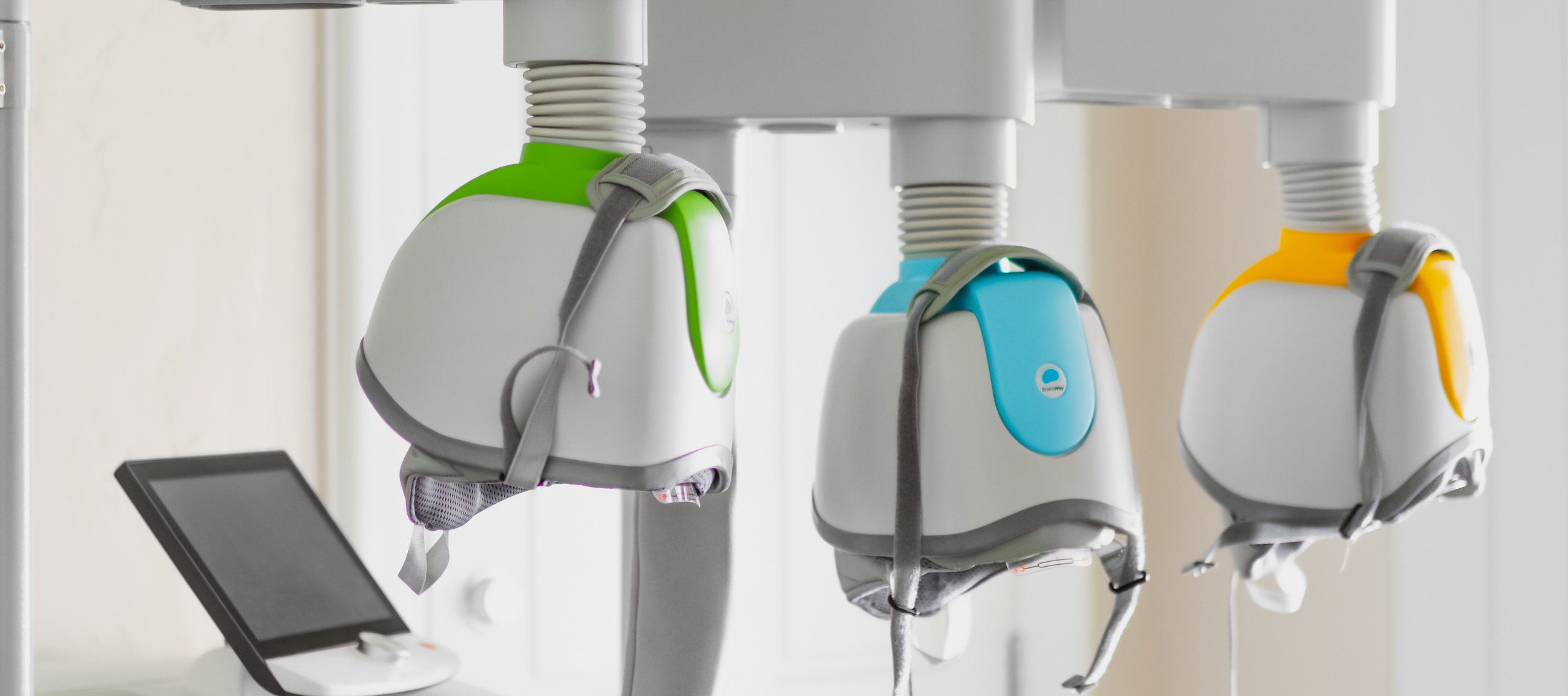
DeepTMS: The Science of Hope for Treatment-Resistant Conditions
For many individuals struggling with Major Depressive Disorder (MDD) or Obsessive-Compulsive Disorder (OCD), traditional “talk therapy” and oral medications sometimes reach a plateau. This is known as Treatment Resistance. At Deva Institute, we bridge this gap using DeepTMS, a non-invasive, FDA-approved breakthrough that talks directly to the brain’s neural circuits.
1. What Makes “Deep” TMS Different?
Standard rTMS (Repetitive Transcranial Magnetic Stimulation) uses a “Figure-8” coil that stimulates the surface of the brain (the cerebral cortex). While effective for some, its reach is limited to about 0.7 cm depth.
DeepTMS uses the patented H-Coil technology, which:
Reaches Deeper: Penetrates up to 4 cm into the brain, reaching critical structures like the anterior cingulate cortex.
Broader Stimulation: It covers a larger volume of brain tissue, reducing the chance of “missing” the target due to minor head movements.
Enhanced Neuroplasticity: By stimulating deeper circuits, it encourages the brain to “rewire” itself more effectively, leading to longer-lasting remission.
2. Clinical Indications: Who is a Candidate?
DeepTMS is not just for depression. At Deva Institute, our multidisciplinary team evaluates candidates for:
Treatment-Resistant Depression (TRD): For those who haven’t responded to at least two antidepressant medications.
OCD (Obsessive-Compulsive Disorder): The first non-invasive device FDA-cleared specifically for OCD.
Smoking Cessation: Helping the brain resist cravings by targeting the reward pathways.
Anxious Depression: Addressing both low mood and the physical symptoms of anxiety.
Deep TMS also effective in these mental and neurological diseases:
Depression, Bipolar Disorder, Panic Disorder, Social Phobia / PTSD, Sleep Problems / Insomnia, Migraine / Chronic Headache, Physical Pain / Fibromyalgia, Parkinsonism, Post-Stroke (CVA), Behavioral problems and various neurological deficits such as difficulty speaking, memory problems, hand tremors, difficulty walking, Excessive and persistent fatigue, Addiction (alcohol, tobacco, cigarette/bidi, hookah, cannabis/charas/bhang, opium, etc.), Mobile / Internet addiction, Gambling addiction, Obesity / Overeating, ADHD, Autism, Ticks / Tourette’s, Memory problem, Dementia, Psychosis and Schizophrenia, Tinnitus (ringing in the ear), Brain fog / Lack of concentration.
3. The Patient Experience: What to Expect
A common fear among visitors is that brain stimulation might be painful or involve “shocks.” This is a misconception.
The Mapping Session: In your first visit, our psychiatrists determine your “Motor Threshold”—the exact amount of energy needed to stimulate your brain.
The Treatment: You sit comfortably in a chair, wearing a specialized cushioned helmet.
The Sensation: You will hear a clicking sound and feel a light “tapping” sensation on your scalp. You can talk to the therapist, listen to music, or watch a video during the 18–20 minute session.
Zero Downtime: Unlike ECT (Electroconvulsive Therapy), there is no anesthesia. You can drive yourself home or go back to work immediately after.
देवा इंस्टीट्यूट, वाराणसी में हम समझते हैं कि मानसिक बीमारी केवल “मन का वहम” नहीं है, बल्कि यह मस्तिष्क के रसायनों और सर्किट की एक समस्या है। जब दवाइयां पूरी तरह काम नहीं करतीं, तब DeepTMS तकनीक काम आती है।
1. DeepTMS क्या है और यह कैसे काम करता है?
DeepTMS एक ऐसी मशीन है जो एक विशेष हेलमेट के जरिए मस्तिष्क के भीतर सुरक्षित चुंबकीय तरंगें (Magnetic Waves) भेजती है।
गहराई तक असर: साधारण मशीनों के मुकाबले, यह दिमाग की उन गहरी परतों तक पहुँचती है जहाँ डिप्रेशन और ओसीडी (OCD) की जड़ें होती हैं।
कोई दर्द नहीं: इसमें न तो सुई लगती है, न ही बिजली के झटके दिए जाते हैं। यह पूरी तरह सुरक्षित और दर्द-रहित है।
2. यह किन मरीजों के लिए सबसे बेहतर है?
ऐसे मरीज जो सालों से डिप्रेशन की दवा खा रहे हैं पर पूरी तरह ठीक नहीं हो रहे।
जिन्हें बार-बार हाथ धोने या एक ही बात बार-बार सोचने की बीमारी (OCD) है।
जो लोग सिगरेट या तंबाकू की लत छोड़ना चाहते हैं।
ऐसे लोग जो दवाइयों के साइड इफेक्ट्स (जैसे वजन बढ़ना या नींद आना) से बचना चाहते हैं।
3. इलाज के दौरान कैसा महसूस होता है?
सेशन के दौरान मरीज आराम से कुर्सी पर बैठता है। आपको अपने सिर पर हल्की “टैपिंग” (जैसे कोई उंगली से थपथपा रहा हो) महसूस होगी। एक सेशन लगभग 20 मिनट का होता है। इसके बाद आप अपनी गाड़ी चलाकर घर जा सकते हैं या अपने ऑफिस का काम कर सकते हैं।
Feature | Medication (Antidepressants) | Standard rTMS | DeepTMS (H-Coil) | ECT (Shock Therapy) |
Anesthesia Needed? | No | No | No | Yes |
Side Effects | Weight gain, nausea, fatigue | Scalp discomfort | Minimal (Mild headache) | Memory loss, confusion |
Depth of Reach | Chemical/Systemic | Surface (Shallow) | Deep & Broad | Whole Brain |
Daily Routine | Minimal impact | Minimal impact | Zero Impact/Walk-in | Requires recovery time |
Frequently Asked Questions (FAQs)
Q: Is DeepTMS the same as “Electric Shock Therapy” (ECT)?
A: No. ECT uses electricity to induce a seizure under anesthesia. DeepTMS uses magnetic pulses (similar to an MRI scan) to stimulate neurons while you are fully awake. There is no memory loss with DeepTMS.
Q: Are there any long-term side effects?
A: Extensive clinical trials have shown no long-term physical or neurological side effects. The most common feedback is a mild, temporary headache during the first week of treatment as the body adjusts.
Q: Can children or the elderly take this treatment?
A: DeepTMS is highly effective for adults and the elderly. For adolescents, our Department of Child & Adolescent Psychiatry evaluates each case individually to ensure it is the most appropriate step.
Q: Who should NOT have DeepTMS?
A: Individuals with non-removable metal in or near their head (such as cochlear implants, brain aneurysm clips, or shrapnel) should avoid TMS due to the magnetic field. Pacemakers are generally okay if the coil is kept at a safe distance, but a prior consultation is mandatory.
Why Choose Deva Institute for DeepTMS?
As an ISO 9001:2015 certified and licensed psychiatric hospital in Varanasi, we don’t just provide the technology; we provide the Expertise.



 Dementia is not a specific disease; it is an umbrella term used to describe a group of symptoms that severely impair memory, thinking, and social abilities, interfering drastically with daily life. It is caused by physical changes in the brain.
Dementia is not a specific disease; it is an umbrella term used to describe a group of symptoms that severely impair memory, thinking, and social abilities, interfering drastically with daily life. It is caused by physical changes in the brain. Psychosis is a severe mental state characterized by a break from reality. When a person is experiencing psychosis, they are unable to distinguish between what is real and what is unreal.
Psychosis is a severe mental state characterized by a break from reality. When a person is experiencing psychosis, they are unable to distinguish between what is real and what is unreal. Depression, clinically known as Major Depressive Disorder (MDD), is a serious medical illness that negatively affects how you feel, the way you think, and how you act. It is not just a temporary case of the “blues” or feeling down after a bad day; it is a persistent change in mood and function that can severely impact quality of life.
Depression, clinically known as Major Depressive Disorder (MDD), is a serious medical illness that negatively affects how you feel, the way you think, and how you act. It is not just a temporary case of the “blues” or feeling down after a bad day; it is a persistent change in mood and function that can severely impact quality of life. A Personality Disorder (PD) is a mental health condition characterized by a persistent and pervasive pattern of inner experience and behavior that deviates significantly from the expectations of the individual’s culture. This pattern is inflexible, starts in adolescence or early adulthood, and leads to distress or impairment in social, occupational, or other important areas of functioning.
A Personality Disorder (PD) is a mental health condition characterized by a persistent and pervasive pattern of inner experience and behavior that deviates significantly from the expectations of the individual’s culture. This pattern is inflexible, starts in adolescence or early adulthood, and leads to distress or impairment in social, occupational, or other important areas of functioning. Addiction is defined as a chronic, relapsing disorder characterized by compulsive drug seeking and use despite harmful consequences. It is considered a brain disease because it causes lasting functional changes to brain circuits involved in reward, stress, and self-control.
Addiction is defined as a chronic, relapsing disorder characterized by compulsive drug seeking and use despite harmful consequences. It is considered a brain disease because it causes lasting functional changes to brain circuits involved in reward, stress, and self-control. Loneliness is not the same as being alone. Loneliness is a distressing subjective experience where a person’s social relationships are perceived as less numerous or less meaningful than desired. It is the feeling of being isolated or disconnected, regardless of how many people are around.
Loneliness is not the same as being alone. Loneliness is a distressing subjective experience where a person’s social relationships are perceived as less numerous or less meaningful than desired. It is the feeling of being isolated or disconnected, regardless of how many people are around.

 Developmental Coordination Disorder (DCD), often referred to as Dyspraxia, is a common neurodevelopmental condition characterized by significant difficulty with the learning and execution of coordinated motor skills.
Developmental Coordination Disorder (DCD), often referred to as Dyspraxia, is a common neurodevelopmental condition characterized by significant difficulty with the learning and execution of coordinated motor skills. Social Communication Disorder (SCD) is a communication disorder characterized by persistent difficulties in the social use of verbal and nonverbal communication. Simply put, the individual struggles with the pragmatics of language—the unwritten rules of social interaction and conversation.
Social Communication Disorder (SCD) is a communication disorder characterized by persistent difficulties in the social use of verbal and nonverbal communication. Simply put, the individual struggles with the pragmatics of language—the unwritten rules of social interaction and conversation. ADHD is one of the most common neurodevelopmental disorders of childhood. It is a brain-based condition characterized by persistent patterns of inattention and/or hyperactivity-impulsivity that interfere with functioning or development.
ADHD is one of the most common neurodevelopmental disorders of childhood. It is a brain-based condition characterized by persistent patterns of inattention and/or hyperactivity-impulsivity that interfere with functioning or development. Disruptive Behavior Disorders (DBDs) are characterized by persistent patterns of angry, defiant, aggressive, and sometimes destructive behaviors in children and adolescents. These behaviors go beyond typical childhood defiance and violate the rights of others and/or significant societal norms, causing serious problems in school, at home, and with peers.
Disruptive Behavior Disorders (DBDs) are characterized by persistent patterns of angry, defiant, aggressive, and sometimes destructive behaviors in children and adolescents. These behaviors go beyond typical childhood defiance and violate the rights of others and/or significant societal norms, causing serious problems in school, at home, and with peers. Communication Disorders are conditions characterized by persistent difficulties in the understanding or use of language, speech, or social communication. These difficulties interfere significantly with a child’s academic performance, social interactions, and ability to participate fully in daily life.
Communication Disorders are conditions characterized by persistent difficulties in the understanding or use of language, speech, or social communication. These difficulties interfere significantly with a child’s academic performance, social interactions, and ability to participate fully in daily life. Feeding and Eating Disorders are serious mental health conditions characterized by persistent disturbances in eating behaviors that significantly impair physical health or psychosocial
Feeding and Eating Disorders are serious mental health conditions characterized by persistent disturbances in eating behaviors that significantly impair physical health or psychosocial